
Shared Insights: the future of interaction between health and social care
In this Shared Insights session, we discussed the future of interaction between NHS Trusts and Local Government amidst a drive for better integrated care; the new Liberty Protection Safeguard legislation due to come into force in April 2022, and the challenges of collaborative working between organisations.
We were delighted to be joined by:
Adam Lent, Chief Executive of think tank New Local, which specialises in advising public services with a network of over 60 local councils.
Mark Barnett, Partner in our Advisory and Inquests team at Browne Jacobson. He advises health and social care providers on issues involving the Mental Capacity Act, deprivation of liberty and Court of Protection applications.
Naomi De Silva, Associate at Browne Jacobson. Naomi specialises in claims against Children’s Services providers and claims under the HRA and DPA.
The Shared Insights were:
Adam Lent set out the increasing need for Local Government and NHS Trusts to work collaboratively in their communities, particularly moving into the post- pandemic era. Budgetary pressures in combination with structure reforms will drive this need.
Historic challenges to collaborative working
- Structural differences between the NHS and local government.
- Differing budgetary pressures.
- Cultural differences between the organisations.
What would make integrated care systems better?
- Local Governments as an equal partner in the integrated care system. Where the NHS works in an egalitarian way rather than taking the lead, local councils have been more optimistic and ambitious in collaborative projects.
- Integration is not just a high-level governance change. Front line staff must be involved in collaborative working to deliver better patient outcomes.
- A cultural change requiring acceptance that the benefits of greater collaboration may not immediately accrue to both organisations equally.
- Using the wider community. Drawing people into a community-led approach to generate more effective social impact.
Mark Barnett set out what we know about the Liberty Protection Safeguards due to replace DoLs in April 2022 following the House of Lords Select Committee report, which concluded the existing Deprivation of Liberty Safeguards (or DoLs) were not fit for purpose, and the Law Commission’s extensive consultation on the law.
The government has published the skeleton legislative framework; however we await the draft Code of Practice. We will hold further session on the Liberty Protection Safeguards in due course once more details are known.
Key differences between the two regimes are:
| Deprivation of Liberty Safeguards (DoLs) | Liberty Protection Safeguards |
|---|---|
| 18 + | 16 + |
| In care homes or in hospital | Applies to all settings |
| Urgent Authorisations | Abolished – but with a different system to authorise in urgent situations |
| Best Interests Assessment | “Necessary and proportionate” assessment |
| Authorisations of up to 12 months | Authorisations of up to 3 years |
| Local Authorities are responsible for authorisations | Local Authorities, CCGs and NHS Trust will be responsible for authorisations depending on where the patient is accessing care |
|
|
Independent scrutiny will be more focused. |
|
|
Greater access to IMCAS |
| Best Interest Assessors | Approved Mental Capacity Professional (AMCP) |
What will not change under the Liberty Protection Safeguards?
- No statutory definition of deprivation of liberty. The ‘acid test’ set out in Cheshire West and Chester Council v P [2014] prevails.
- Assessment will include the patient’s capacity as defined by the MHA 1983.
- Right to appeal an authorisation remains with the Court of Protection (non-means tested legal aid funding is retained).
- MHA 1983 interface remains in place, whilst some of the statutory frameworks overlap they do not all dovetail.
Expected Process for Liberty Protection Safeguards – DHSC flowchart:
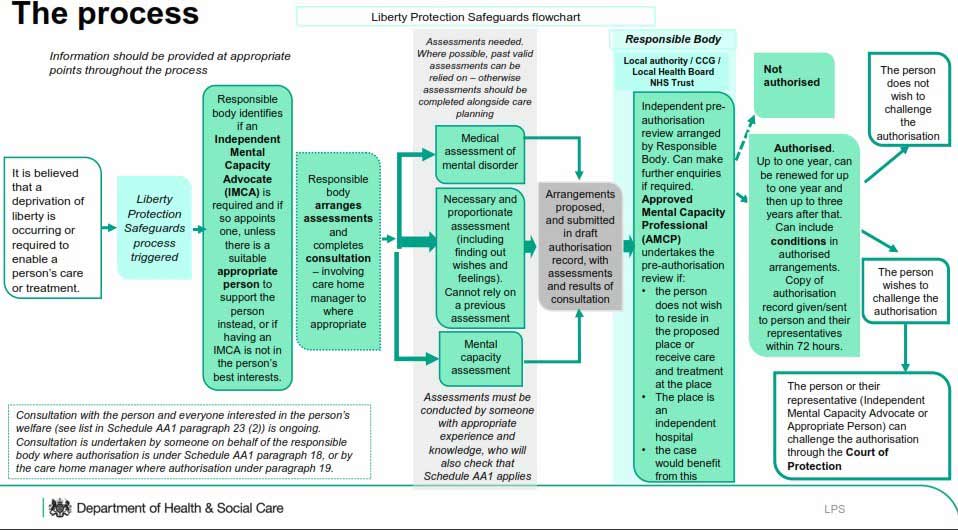
Naomi de Silva outlined that often there can be limited collaboration between Local Authorities and NHS organisations in matters involving care proceedings.
- Care proceedings involve the safeguarding of children and are highly sensitive. Proceedings are held in private with no public reporting.
- Clinicians may be asked to provide statements with limited or no information about the case from the LA who are often wary of disclosing privacy rules by sharing information.
- Requests for statements are often urgent or last-minute and clinicians have limited/no training on drafting statements.
What can Trusts do to help Clinicians?
- Clinicians can sometimes be caught unawares by criticisms in an expert report which can cause distress and reputational issues. Ensuring clinicians understand what the case is about before they give evidence is key to helping clinicians prepare adequately.
- Consider whether a clinician needs legal representation. Is there likely to be aggressive questioning of a clinician?
- Engage with the children’s legal team at the LA as early as possible to understand what is going on and what is needed from the statement. Developing good working-relationships with key personnel at the Local Authority can help with this.
- Make it clear a statement is factual, based on the records and that whilst some opinion on how an injury was causes is permissible the statement should make clear what is fact and what is opinion.
- If the LA are resistant to sharing information keep pushing for it. There is case law for to compel the Local Authority to give limited disclosure where clinicians are giving evidence as experts which can be drawn on when giving factual statements (see W (A Child), Re [2016] EWCA Civ 1140 (17 November 2016) (bailii.org) Paragraph 95)
During the discussion, key themes emerged including planning for the implementation of LPS with limited information regarding the detail which is still awaited, collaboration including pooling resources such as AMCPs and dealing with requests for statements from clinicians.
Speakers


Naomi De Silva
Associate
Shared Insights
Our monthly forum connecting health and care leaders and professionals to discuss challenges and share solutions.
Contacts

Mark Hickson
Head of Business Development
onlineteaminbox@brownejacobson.com
+44 (0)370 270 6000

Nicola Evans
Partner
Nicola.Evans@brownejacobson.com
+44 (0)330 045 2962



































