Employment & Workforce Survey 2021: Vaccinations in the workplace
Covid vaccinations remain a particularly charged topic, with strong feelings held by both those pro- and anti-vaccination.
Covid vaccinations remain a particularly charged topic, with strong feelings held by both those pro- and anti-vaccination. With the Government largely advocating vaccination by encouragement rather than through mandates (although see below for the different approaches taken within health and social care in England), employers have grappled with whether a “no jab – no job” policy can be adopted. Others have considered whether to link returns to work premises with proof of vaccination – requiring those who are unvaccinated to continue working from home.
For those employer who wish to encourage vaccination, a link to the Government’s vaccination guide for employers can be found here. Acas guidance can also be found here.
Can employers insist on Covid vaccination?
No employer can lawfully force an employee to be vaccinated – the issue instead is whether the employer can refuse to employ someone who is unvaccinated, or can take disciplinary action and/or dismiss an existing employee if they refuse to comply with a policy of mandatory vaccination.
There are different risks of mandatory vaccination depending upon whether an employer is seeking to impose the requirement on its current workforce, or on new employees only. There are also different risks depending upon the nature of the employer and the work undertaken – and, in particular, whether they fall within the different provisions applicable to care homes or the new proposed wider health and social care provisions (see below).
Claims could include discrimination allegations from staff (or applicants) who have decided not to have the vaccination (for example on religious grounds, health grounds or because they are pregnant) and feel that their personal views and/or beliefs or health has not being considered. If existing staff refuse to be vaccinated and are dismissed as a result, this could lead to claims for unfair dismissal (if they have the required 2 years’ service).
In view of these risks (particularly combined with the approach taken more generally in the UK to keep vaccination as a matter of personal choice), it is unsurprising that many employers have not gone further than encouraging vaccine uptake. Our recent survey indicates that the vast majority of responders (over 80%) are not insisting on compulsory vaccinations for any reason.
Are you considering requiring evidence of vaccination status at all?
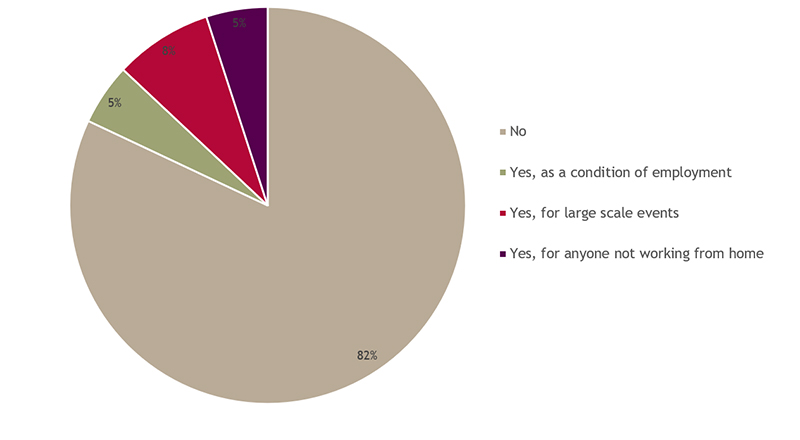
Those that were asking for evidence of vaccination status were from a range of sectors – including health, manufacturing and industrials and government. There were no clear links between whether or not evidence of vaccination status was requested and the availability of enhanced contractual sick pay.
Vaccinations, self-isolation and sick pay
Enhanced contractual sick pay was generally viewed by responders as of low importance to staff retention. Our question asked responders to rate the importance of enhanced sick pay to staff retention with 1 being the most important, 5 being the least important. Enhanced sick pay received the highest number of category 5 votes. It, together with “other benefits” made up the vast majority of combined category 4 and 5 votes (just shy of 80%).
However, issues have arisen following the changes to the self-isolation requirements for those who are vaccinated (introduced in August 2021). For example, the type and amount of pay for those who are required to self-isolate due to close contact (where the individual themselves is not ill) is a question that many employers are asking. Also, employers are asking if self-isolation periods should be treated as sickness absence for the purposes of absence management. (Just to be clear, self-isolation absences would still fall within the SSP regime as per the government’s guidance, assuming the other qualifying requirements are met.)
Whilst the majority of responders (58%) offer enhanced contractual sick pay to their employees, over 10% indicated that their enhanced sick pay offering had been, or was being, amended due to the changes to the self-isolation requirements. Again, responders falling within this category were from a range of sectors; however, half were either from education or local government sectors.
The self-isolation requirements changed in November 2021 – requiring all close contacts with the Omicron variant to self-isolate, regardless of vaccination status. However, with effect from 14 December 2021, the distinction between vaccinated and unvaccinated where there has been close contact with someone who has tested positive has been reinstated once again. Those who are vaccinated are not required to self-isolate due to close contact but instead must undertake daily testing for a period of 7 days. Those who are unvaccinated are required to self-isolate for 10 days. How such self-isolation absences should be treated is therefore likely to be a continuing issue for employers.
Health and social care - Care Homes
The Health and Social Care Act 2008 (Regulated Activities) (Coronavirus) Regulations 2021 were made on 22 July 2021 and came into force on 11 November 2021. It is now a legal requirement to restrict access to CQC-regulated care home premises in England to those who have not received a full dose of an authorised Covid-19 vaccination, unless one of the limited exemptions apply.
Exemptions apply to:
- Residents;
- Those who have medical exemptions;
- Friends and family of residents who are visiting;
- Those under 18;
- Those attending in the execution of their duties as a member of the emergency services;
- Those entering to assist in an emergency or to provide urgent maintenance work;
- Those who are visiting a service user who is dying; and
- Those who are visiting a service user to provide comfort or support in the event of a bereavement.
There are very few medical exemptions which will apply – examples include those who have had an allergic reaction to a previous dose of the vaccine, or any of the vaccine components. Time-limited exemptions may apply for those with short-term medical conditions or who are pregnant, should they wish to take it.
It is possible for individuals to self-certify that they meet the medical criteria for exemption. A specific self-certification form is available on the Government website. However, self-certification will only be possible for a limited period of time. Initially, this was to be available until 24 December 2021 but due to delays in the formal certification process, this has been extended to 31 March 2022. All those who self-certify before 24 December will have until 31 March to secure formal proof of their medical exemption status. The extension letter is clear that from 1 April 2022, proof of a formal medical exemption or full vaccination against COVID-19 will be required in order to comply with the Regulations and continue working in a CQC-regulated care home.
There is a specific process for seeking a NHS COVID Pass to formally prove medical exemption – including first requesting an application form by telephone only. Once the form has been completed and returned, guidance indicates that results will be posted 2 to 3 weeks after applying.
Pregnant women can instead rely on their MAT B1 certificate; the exemption will, however, expire 16 weeks after childbirth.
Wider health and social care
The Government has also announced its decision to move ahead with compulsory COVID-19 vaccinations for certain health and social care staff working in England. Steps are proposed to be introduced with effect from 1 April 2022, following concerns that a more immediate push for compulsory vaccinations might place too much pressure on health and social care provision and a potential staff exodus during the always challenging winter months.
The Government’s proposed approach to put the requirements on a statutory footing is through an amendment to the Health and Social Care Act 2008 (Regulated Activities) Regulations 2014. Providers of CQC regulated activities will only be allowed to deploy individuals who have been fully vaccinated against COVID-19 (or who are exempt) to roles where they interact with patients or service users. This is wider than “frontline” staff as it will include other non-clinical workers who have face to face contact with patients – such as receptionists, ward clerks, porters and cleaners.
The proposed Regulations will apply in health and social care settings including hospitals, GP practices and where care is delivered in a person’s home. They will apply to CQC-regulated activities whether they are publicly or privately funded. They will also apply where the regulated activity is delivered through agency staff, volunteers or trainees, or contracted to another provider.
This is a different approach to that taken in respect of care homes where, as set out above, the obligation relates to those entering the premises of CQC regulated care homes and is not simply limited to those persons undertaking direct treatment or personal care as part of the carrying on of a CQC regulated activity.
Guidance from NHS England and NHS Improvement published on 6 December 2021 to assist healthcare employers to prepare can be found here.
If you would like discuss the impact of any of the issues raised above on your organisation, please feel free to contact Emma Hughes.
Contact

Emma Hughes
Partner
emma.hughes@brownejacobson.com
+44 (0)330 045 2338






























